Cutting Through The Remote Patient Monitoring Hype
By Jim Pomager, Executive Editor
Sometimes it’s difficult to separate hyperbole from reality when it comes to remote patient monitoring (RPM) and its potential impact on healthcare.
On one hand, there is a ton of hype surrounding RPM and related industry buzzterms like wearables, mobile apps, big data, the Internet of Things (IoT), and mHealth. Extensive — arguably excessive — mainstream and trade media coverage of the technology is only fanning the flames. (In the spirit of full disclosure, Med Device Online is not entirely above reproach.) Check out this sampling of recent headlines:
- Remote Patient Monitoring Market to Top $26 Billion by 2018
- Apple, Google, Samsung May Combat Diabetes with Wearables
- Can Data From Your Fitbit Transform Medicine?
- The mHealth Movement: The Rise of Connected Home Medical Monitoring Devices
On the other hand, to some degree the hype is justifiable. RPM has the potential to significantly improve the efficiency and efficacy of healthcare. It is already providing new ways to aggregate patient data from outside the confines of the healthcare facility, and to communicate that information to the clinical community — wherever, whenever, and however they need it. It can help move patients from the hospital to home more quickly, reduce hospital readmissions by having patients play a more active role in their recovery, and identify problems (and potential problems) before they become major episodes. As such, RPM could play an important role in attaining the holy grail of modern healthcare: simultaneously improving care and reducing costs.
Plus, a series of technological advances have paved the way for medical device and diagnostics companies to become more involved in RPM, making it easier for them accelerate its adoption and reap the rewards of its ultimate success. For instance, there’s the continuing proliferation of mobile devices. This phenomenon has not only put a potential medical data collection/communication tool in the hands of almost every patient in the developed world, it has also driven down the cost, size, and power requirements of sensors, radios, and other electronics that can be integrated into medical devices and diagnostic equipment. The space is ripe for medtech innovation.
At the MD&M East conference last month, a group of RPM experts gathered to discuss the hysteria, challenges, and opportunities surrounding RPM during a panel session titled The Journey of Remote Patient Monitoring. What do medical device makers need to do to take advantage of this trend? How do wearables fit into the RPM equation? Should the medtech industry fear or embrace the involvement of tech titans like Google and Apple in the movement?
Read on for answers to these and other important questions concerning the remote patient monitoring revolution.
Embracing The Big Data Opportunity
Back in 2010, Eric Schmidt of Google famously claimed that human civilization had produced 5 exabytes (5 billion gigabytes) of data between the dawn of civilization and 2003, and that by 2010, we were producing that much information every two days. With the advent of the IoT, the already “big” amount of data being generated will grow exponentially in the coming years. According to a recent report by market research firm IDC, the IoT currently comprises some 20 billion connected “things” — all of them collecting, sharing, and/or using data — and that number is expected to approach 30 billion by 2020. “I don't know if the term should be ‘big data,’ as opposed to ‘huge data,’” Byron Mattingly, Ph.D., chair-elect of the American Society for Quality’s (ASQ’s) Software Division, quipped during the panel session.
Why is this relevant for medtech companies? Because there is a ton of information available to leverage and incorporate into medical devices that are more useful in managing patient health.
When people think about RPM data, they usually envision physiologic measurements taken by sensors attached to or implanted in a patient. And while this data is fundamental to RPM, all kinds of other information is being collected that can help form a more complete picture of a patient’s health and risk factors. For example, accelerometers in wearable devices can track the activity level of a patient throughout the day, indicating how much they walked around the house, went up and down the stairs, and slept. Readily available environmental data can also play an important role — weather, temperature, and pollen count information can be critical in managing respiratory conditions like asthma, for instance.
“The discoveries of tomorrow are embedded somewhere in this goliath set of information that is big data, though people often gloss over the promise of today,” said Andrew Malcolmson, director of Covidien’s Integrated Patient Intelligence business, whose virtual patient monitoring platform enables continuous remote patient monitoring via web-connected devices. “Some of these tools, these communications present an opportunity to make practice better today based on what is known, while preparing to make a better tomorrow based on what is not.”
3 Remote Patient Monitoring Challenges That Medtech Companies Must Address
The amount of data and size of the opportunity may be great, but the medtech industry still has some considerable obstacles to overcome to achieve success in RPM. Here are three outstanding challenges the panelists identified:
1. Providing meaningful data
Perhaps the biggest struggle for device makers is figuring out a way to filter the massive amounts of available data, so that what they deliver to patients and providers is digestible, meaningful, and actionable. Patients need what Malcolmson called “situational awareness” — information that helps them visualize the ramifications of their current behavior and recognize a path to improvement. And providers want a clear understanding of what’s really going on with the patient, either early in the onset of a condition or (ideally) in advance, so they can provide a plan to prevent it.
“The challenge for us is not so much that there's a lot of data,” said Todd Thompson, VP of corporate development at Proteus Digital Health, which has developed a system that combines ingestible and wearable sensors to provide real-time information about medication-taking, rest, and activity. “The challenge is that doctors and patients don't want big data. What they want is information that they can actually use to actually make changes.”
In many cases, the information you don’t provide is as important as the information you do. Devin McCombie, Ph.D., VP of science and research at Sotera Wireless — a developer of wireless, body-worn vital sign monitoring technology — brought up the issue of false alarms and their effect on patients. “If we start alarming or alerting the patient too much, it actually bothers them and they’re not going to be compliant,” he said. “It can actually scare them, and that’s not something we want.”
McCombie also said you need to be careful about providing nothing but bad news. “Do you really want to put on a sensor to see how unhealthy you are?” he asked, referring to wearable medical devices. “If it's just going to give you bad news, you may not want to use it,” he added. That’s something we really do have to work on, where we're not just giving people that bad news but actually presenting them with data in a way they can take action on.”
2. Making the sensors “disappear”
Just as patients (and doctors) want to remain unaware of all but the meaningful, actionable data, they also want to forget about the fact that they are carrying around a RPM device. For the next generation of patient sensors to succeed, the panel agreed, they must be truly wearable — unobtrusive, tolerable … almost invisible to the person transporting them around.
“Sensors will never engage patients, and neither will remote monitoring,” Proteus’ Thompson explained. “We have to, as technology companies, do our best to make the sensors disappear into the background.” Sensors should be nothing more than “enablers,” he said, collecting information that is valuable and can later be used to engage patients.
“At Covidien, we believe that one of the keys is to make the measurement devices go away,” Malcolmson concurred. “The key to active patient engagement and data generation, for the most part, is to not have to have the patient engaged, but to make the device automated, just streaming the information that's necessary.”
3. Keeping the patient engaged
Although patient engagement in sensors and data gathering should be minimized, their engagement with the information collected and filtered by those sensors should be maximized. The panelists expressed that one of the key factors in designing an RPM device is striking a balance between moving the technology to the background and keeping patients suitably engaged.
“Sometimes the patients want to interact with their devices because of the feedback, because it gives them that minty fresh tingle,” ASQ’s Mattingly pointed out. He then used an illustration from the consumer products space: “When Procter & Gamble was trying to market Febreze [odor eliminator], they had a great difficulty marketing it, because it lacked that fresh smell. They subsequently had to add more scent to Febreze, so that people would know that their sheets and pillowcases and couches were now clean.”
“If the tool provides you with information that helps you to use positive behaviors and actually reinforces those positive behaviors, and then you see those behaviors having an effect on how you feel, how you're able to live, and how much you can move around and interact with your family — that's what's important,” Thompson said.
The trick is determining the proper balance for your technology and the patients in its specific treatment area. “I think the interactive aspect cannot be ignored, and the question will be: Which things do we want quietly monitoring in the background, and which things do we want interacting with us?” Mattingly said.
How Wearables Fit In
The panelists agreed that wearables will play a crucial role in helping move patients out of healthcare facilities more quickly, monitor recently discharged (and chronically ill) patients, and prevent admissions/readmissions. Their potentially huge economic impact on healthcare has drawn attention from hospitals, payers, and even traditional medical device makers. For example, Covidien recently raised its stake in remote patient monitoring by acquiring wearables developer Zephyr Technology.
Sotera’s McCombie foresees a future in which wearables become omnipresent in healthcare. “You can actually see wearable monitoring start from the very first engagement, with the ambulance,” he said. “The monitor can then travel with the patient throughout their continuum of care and be released with them when they go home.”
However, tomorrow’s RPM wearables likely will not be today’s health wearables. Thompson doesn’t see a big place for the Fitbits and the Nike Fuels of the world in healthcare. “They are not healthcare companies, and they are collecting, some would argue, marginally useful information. They are expensive pedometers. They're cool, they're nice to look at it, but they’re pedometers,” he said. “Wearables are going to be important, and the other sensors as well, but they have to provide meaningful information, information that actually pertains to the disease or the chronic illness at hand — not just how many steps you took in a day.”
Apple, Google, Samsung — A Device Maker’s Friends Or Foes?
Each of the panelists expressed unabashed enthusiasm around the involvement of tech titans like Google, Apple, Samsung, and others in the healthcare space, saying that it will only accelerate the advancement of RPM technology.
For one, these electronics companies have supplied the world with the perfect patient engagement tool: the smartphone. Almost everyone owns one of these sensor-laden, sophisticated computing and communication devices, and they already use and love them — a lot. “The key to patient engagement is taking advantage of things that we already use, the tools that Apple and Google and Samsung have created, which are these amazing patient engagement tools,” Thompson said. “We just have to provide applications that show the information.”
“I think what they're doing, which none of us in the medtech world could ever do, is creating marvelous hubs for data collection, data transmission, and information display,” Thompson added. “They are the interface, the engagement tool, that we are all going to use, and they are actually making changes to their operating systems to improve our ability to do that, and that's what is exciting.”
And medtech companies can now innovate on top of these incredible platform technologies. “Our forte, our strength, is not in systems development, but we do have good ideas and a strong relationship with the clinical community. So this gives us the opportunity to offload some of that developmental overhead and focus on the things that we really do well,” Covidien’s Malcolmson explained. “Additionally, it allows the innovators, the startups, the entrepreneurs out there to have their ideas see the light of day. If they were encumbered by having to develop this platform system in order to deploy their solution, it just wouldn’t happen.”
Finally, Google, Apple, and Samsung also lend their considerable reach, which can generate far more awareness of and demand for remote patient monitoring than medtech companies could ever hope to deliver on their own. “Once you become acutely aware of what remote monitoring can do, wouldn't you look to your hospital to see if they have that type of capability?” Sotera’s McCombie asked. “Wouldn't you choose the hospital that has it? So it can really work on paper and drive the marketing for us.”
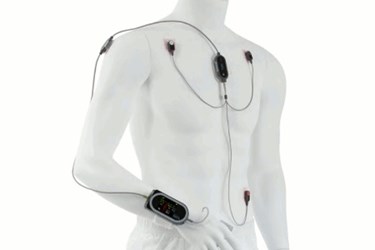
Image of ViSi Mobile System courtesy Sotera Wireless
