Know Your Market: Leverage Data Transparency To Inform Precise Patient Journey Models
By Michelle Edwards and Bill Woywod, Navigant Consulting, Inc.

To find and serve intended patients, medical technology and pharmaceutical companies tend to set their go-to-market strategies using basic claims data, as well as patient and provider insights. Much of this information is gleaned from voice-of-customer analysis, generously laced with confidence in the technology’s prowess. In the process, companies typically invest millions of man-hours and dollars, only to fall short of their market expectations.
Today, these kinds of educated approximations and high-stakes speculations are outdated, giving way to extract precise insights.
Commercial and government-sponsored payers, including Medicare, are publishing comprehensive claims-based data sets to help promote transparency across the healthcare industry. This enables payers and regulators to see costs more easily, and puts the onus on manufacturers and providers to use the data to demonstrate cost-effectiveness and positive outcomes. This shift also benefits consumers indirectly, as it supports the industry’s shift toward value-based care initiatives that base reimbursement on provider quality and patient outcomes.
For medtech and pharmaceutical companies, this data provides unparalleled insight into clinical practice care pathways.
The patient journey is unique to each patient, but organizing these journeys according to macro-level similarities for a given condition can characterize interaction between patients, providers, and payers in real time to inform key stakeholder decisions.
Data sets from Medicare and commercial claims databases provide a representative sampling of the majority of people in the United States. Missing segments can be filled with data-driven estimations. These relevant data sets can be leveraged in combination with 1) on-point query and analysis design, 2) skilled programming, and 3) deep industry expertise to conduct longitudinal data analysis that leverages years of data to provide a precise understanding of patient journeys in the healthcare system.
As a result, companies can pinpoint opportunities for therapy intervention and create far more effective market development and commercialization strategies.
Overcoming Common Barriers to Adoption
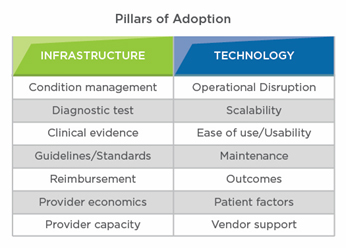
Precision patient journey mapping helps companies uncover critical barriers to adoption. For example, if and when a patient presents for treatment depends on how much the condition “bothers” the patient — which can vary largely based on the individual’s own threshold for pain or discomfort, ability to make lifestyle adjustments to minimize a condition’s affects, and knowledge of available treatment options.
Consider back pain: some people will simply avoid activities that exacerbate their pain, while others might self-administer over-the-counter drugs or seek medical attention. If your company had an innovative surgical intervention, you would want to fully understand the number of patients present for diagnosis, where to find them in the clinical care pathway and, just as importantly, where they do not present.
Traditionally, a patient journey rendering might look like Fig. 1, which details clinicians a person with back pain might seek out. However, Fig. 1 fails to drill down into the point in that patient’s treatment-seeking journey where they would visit a clinician, or how influential these providers are in prescribing a specific interventional surgery.
Fig. 1 — Traditional Patient Journey
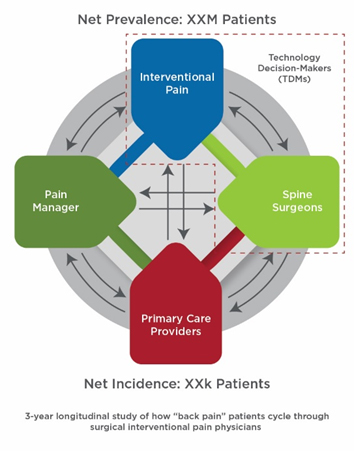
However, if you leverage 70,000 patient records to track longitudinal movement across provider segments, you will know exactly where patients present (Fig. 2):
Fig. 2 — Data-rich Patient Journey Mapping Pinpoints “Sweet Spots”
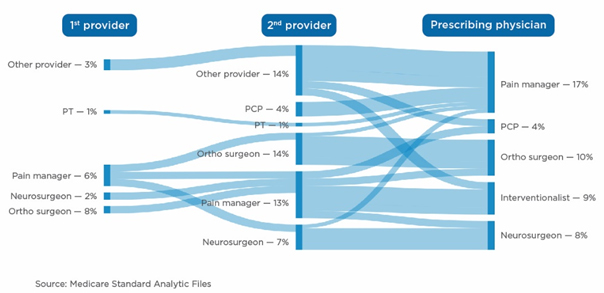
In this example, analysis revealed the prevalence pool (i.e., patients seeking treatment) moves frequently through the system on a year-to-year basis. Of those, 70 percent who visit an interventional pain or spine surgeon are new patients each year, and this pool of patients uses significant resources, with an average of five visits per patient per year. Using this data, a pattern of visit trends emerged, revealing an opportunity to intervene further upstream in the care continuum, which would allow for a reduced number of total visits, as well as an opportunity to avoid more clinically invasive and expensive procedures later.
Another common patient-journey-oriented adoption barrier resides within condition diagnosis. Generally, for any given condition, there exists a certain — sometimes significant — percentage of undiagnosed people. Finding these people and compelling them to seek treatment creates a win-win: the company breaks into an untapped market, and the undiagnosed patients gain knowledge of and access to a potential treatment.
Recently, a global durable medical equipment provider solicited research regarding the market size of a pulmonary chronic disease. Using the comprehensive body of available research, including an in-depth analysis of large healthcare claims data sets, researchers revealed an additional four million people than had been previously known — a 25 percent increase in the potential market representing millions of dollars.
In another case, a pharmaceutical company with a peripheral arterial disease treatment option initially planned to focus its efforts on physicians who treated co-morbid diabetic patients. Based largely on prior experiences and discussions with key opinion leaders, the company believed these patients were evenly distributed across several physician groups treating conditions associated with diabetes (e.g., medical ophthalmologists, retina specialists, and endocrinologists). However, deeper analysis revealed a much different reality (Fig. 3).
Fig. 3 — Finding the Right Audience
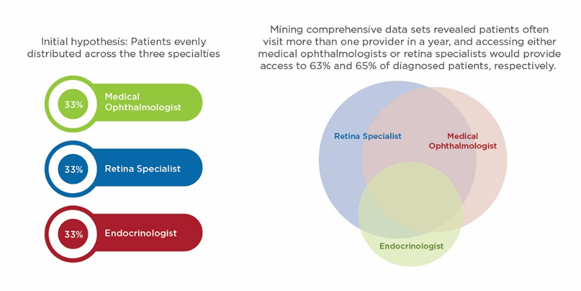
These patients actually saw more than one of these specialists annually and, as such, targeting medical ophthalmologists or retina specialists alone would enable the company to reach just two-thirds of its potential patients — a strategy that warranted a distinctly different market strategy.
Avoiding Major Risk and Repercussions
Patient bother, condition diagnosis, and the referral dynamic are just three of the 14 critical adoption barriers companies face when launching a new device or drug therapy. When a company fails to truly understand its intended market — especially where and how to reach its intended users — it is exposed to a variety of serious risks, including wasting significant time and resources pursuing the wrong patients or providers.
Unfortunately, many companies continue to rely on outdated data-collection and analysis practices, including voice-of-customer and simple claims data, to create their patient journey scenarios. The problem with these practices is they lack comprehensive data and long-term perspective.
Voice-of-customer research tends to enlist a network of known patients, and therefore fails to account for the experiences of those who remain undiagnosed or untreated. This type of research also tends to backfill a predetermined narrative, such as when a company with a varicose vein treatment option interviewed its patients — white, affluent women of a certain age seeking treatment for largely cosmetic reasons — who happened to represent a saturated part of the market. While the findings were accurate to this group, they completely overlooked an untapped segment identified later through research (i.e., a significant candidate pool, largely men, who remained untreated for varicose veins and associated painful ulcers).
Similarly, traditional claims data is inherently limited. The results of claims data are gleaned from the four diagnosis code slots that providers fill in, based on their knowledge at the time, to satisfy payers. In other words, traditional claims data provides a limited snapshot that misses unassociated conditions or ensuing trends emerging over time.
In contrast, fully leveraging comprehensive data sets allows you to track patient treatments over time, providing a more accurate view of the patient journey, as well as discerning any related conditions, characteristics, or milestones.
Thanks to this increasing data transparency, the precise patient journey is now knowable. It requires advanced data analysis tools and computational expertise, with access to both published and licensed data sets, to create validated patient journey maps. It’s a proven way to identify exactly who to target, where, and when, that will equip your team to confidently determine and implement the most effective strategies for market development, market access, and commercialization.
About The Authors
Michelle Edwards is a Director in the Life Sciences practice at Navigant. She has nearly 20 years of experience in life sciences, with roles in asset valuation, business development, finance, investor relations and marketing. Her work at Navigant is focused on market development strategy and tactical, local, market development planning. Most recently she has worked on projects in therapeutic areas including ophthalmology, hematology, oncology, orthopedic, peripheral vascular intervention and emergency medicine.
Bill Woywod is a Managing Consultant in the Life Sciences practice at Navigant, where he leads big data analytics and machine learning projects. He has played a central role in expanding Navigant’s deep data analytics capabilities, including the development and execution of sophisticated claims data analyses and machine learning initiatives for clients in the medtech and biopharma industries. Previously, Bill worked as a data scientist at a large regional health plan, where he led the development and successful execution of the organization’s first machine learning program.
