Microscopic "Obstacle Course" Reveals Insights Into Metastasis
By Chuck Seegert, Ph.D.
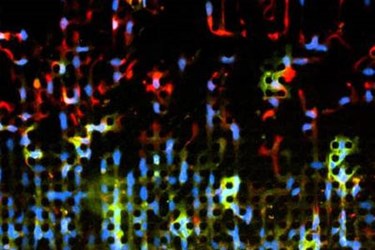
Researchers at Brown University may have gained some insight into how cancers can rapidly metastasize and spread through the body using a microchip model system. The interesting results of their work may speed research into ways of halting metastatic development in its tracks.
A major area of concern in cancer progression is the development of metastases, or daughter tumors that crop up in other areas of the body. It is thought that this metastatic spread is caused by a mechanism known as the epithelial-mesenchymal transition (EMT).
EMT is a cellular phenomenon that allows epithelial cells like the ones that coat the surfaces of organs, blood vessels, and even the skin to transition into a cell with mesenchymal properties. Mesenchymal cells are the cells that form the connective tissues in the body like muscle, tendons, and bone. What’s different about this cell type is its ability to move as a single cell, while epithelial cells are more social and require groups of cells that adhere to one another for their normal function.
While it is known that cancer invades surrounding tissues, thus involving them in the disease, insight into how this happens remains elusive. In a recent study published in Nature Materials, however, a Brown University team may have shed some light.
"People are really interested in how EMT works and how it might be associated with tumor spread, but nobody has been able to see how it happens," said lead author Ian Y. Wong, assistant professor at the Brown School of Engineering and the Center for Biomedical Engineering, in a recent press release. "We've been able to image these cells in a biomimetic system and carefully measure how they move."
Wong performed the research as a postdoctoral fellow at Massachusetts General Hospital.
To make this advance in understanding, the Brown University team turned to micromachining methods like those used to manufacture silicon wafers to make microchips. Once microarrays had been machined on the surface of the wafers, they were used as molds to cast polydimethylsiloxane (PDMS) substrates for cells to be cultured on. According to the press release, the features used were pillars with 10 micron diameters organized in arrays with 10 micron spacing.
The matrix developed by the Brown university team provides a way of seeing how cells react in a situation that provides barriers like those seen in vivo.
"It's basically an obstacle course for cells," Wong said in the press release. "We can track individual cells, and because the size and spacing of these pillars is highly controlled, we can start to do statistical analysis and categorize these cells based on how they move."
Epithelial cells were placed on the substrates and then manipulated chemically to induce them to act more like malignant, mesenchymal-type cells. The majority of the cells retained their normal behavior, but according to the press release, some 16 percent started to move quickly through the obstacle course-like matrix. The 84 percent of cells that remained were relatively static and continued to express markers that indicated they were epithelial in origin, while the fast moving mesenchymal-like cells showed a reduced sensitivity to drugs applied in the culture.
"That was a remarkable result," Wong said in the press release. "Based on these results, an interesting therapeutic strategy might be to develop drugs that downgrade mesenchymal sports cars back to epithelial economy models in order to keep them stuck in traffic, rather than aggressively invading surrounding tissues."
Cell behavior is an interesting method of understanding metastatic cancer development. An article recently published on Med Device Online reports on another approach to understanding cancer cell migration.
Image Credit: Ian Y. Wong / Brown University
