Owlstone Medical Receives CE Mark Approval For Pediatric Disease Breathalyzer
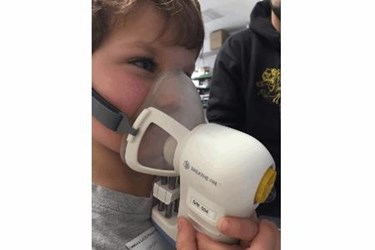
Extends ReCIVA technology deployment in MRC EMBER project for use in acutely breathless children and asthmatics
Owlstone Medical, a diagnostics company, recently announced it has developed and received CE mark approval for a paediatric version of the company’s disease breathalyzer, ReCIVA. The marking extends the scope of breath testing in early stage diagnostics and therapy response to include children and in particular, the difficult to manage group of child asthma patients. Both the adult and pediatric versions of the breathalyzer are now being used in EMBER (East Midlands Breathomics Pathology Node), a £2.5M project, funded by the Medical Research Council (MRC) and the Engineering and Physical Sciences Research Council (EPSRC). The primary aim of EMBER is to develop breath-based systems for molecular pathology of disease and clinically validate breathomics as a new diagnostic modality.
Currently one in 11 children in the UK has asthma and it is the most common long-term medical condition. Volatile organic compounds (VOCs) in breath have been shown to correlate to inflammatory subtype in asthma, which helps guide better treatment decisions. Owlstone Medical uses the Respiration Collector for In Vitro Analysis (ReCIVA), in combination with the Field Asymmetric Ion Mobility Spectrometer (FAIMS) sensor platform, to accurately and selectively detect volatile organic compounds (VOCs) in breath. In February, the company won an NHS contract for STRATA (Stratification of Asthma Treatment by Breath Analysis) to adapt its disease breathalyzer technology for precision medicine and companion diagnostics in asthma. The paediatric version of ReCIVA is suitable from ages 5 and up and has been developed as breath sampling offers a completely non-invasive way to test children.
EMBER was established by the MRC and EPSRC as an academia/industry consortium to develop breath-based systems for molecular pathology. EMBER draws upon expertise in clinical research, analytical chemistry, data management and mathematical modelling of complex data across the East Midlands to develop rapid, near patient non-invasive approaches to diagnosis, phenotyping and stratification.
Billy Boyle, co-founder and CEO at Owlstone Medical commented: “Managing the diagnosis and treatment of children presenting with asthma and severe breathing difficulties is often problematic. Breath analysis presents a significant opportunity to better predict how a child will respond to certain treatments, including steroids and expensive biologics. In developing a paediatric breath sampler we are expanding the scope of projects such as EMBER to include children as an important group in the study of asthma, and more generally extending other biomarker and discovery studies using breath.”
Professor Chris Brightling, EMBER and Leicester NIHR Respiratory Biomedical Research Unit Director, Professor in Respiratory Medicine at University of Leicester, Precision Medicine Institute added: “Choosing the right treatment for the right patient is especially challenging in children as obtaining samples such as blood to measure disease activity can be difficult. Breath analysis offers an excellent opportunity to sample the airway by simply breathing into a mask. This presents a new approach to understand disease and make better treatment decisions”.
About Owlstone Medical
Owlstone Medical has developed a breathalyzer for disease. With a focus on non-invasive diagnostics for cancer, infectious disease and inflammatory disease, the company aims to save 100,000 lives and $1.5B in health care costs by 2020.
The company’s microchip FAIMS (Field Asymmetric Ion Mobility Spectrometer) sensor is a platform technology that can be programmed in software to detect targeted biomarkers of disease in breath (and other bodily fluids). FAIMS can be used in clinical diagnostics and precision medicine with application in cancer and a wide range of other medical conditions. Highly sensitive and selective, these tests allow for early diagnosis when treatments are more effective and where more lives can be saved.
Owlstone Medical is currently developing tests for lung and colorectal cancer, two of the most common cancer killers worldwide. The company also sells R&D tools and services to academic, clinical and pharma partners who want to develop breath based diagnostics for their own applications.
Founded in 2004 as a spin-out from the Engineering Department at the University of Cambridge University, Owlstone Inc is a profitable business selling it’s proven FAIMS technology to military and industrial customers globally. Owlstone Medical was spun out from Owlstone Inc in 2016 to develop and commercialise FAIMS in diagnostic applications.
Owlstone Medical is headquartered in Cambridge, UK, with offices in London, UK. For more information, visit www.owlstonemedical.com.
About The East Midlands Breathomics Pathology Node (EMBER)
As one of six Molecular Pathology Nodes, the East Midlands Breathomics Pathology Node (EMBER) has been established with a £2.5M grant from the Medical Research Council (MRC) and the Engineering and Physical Sciences Research Council (EPSRC) to develop breath-based systems for molecular pathology.
EMBER draws upon expertise in clinical research, analytical chemistry, data management and mathematical modelling of complex data across the East Midlands from University of Leicester, University Hospitals of Leicester NHS Trust and Loughborough University together with industry to develop rapid, near patient non-invasive approaches to diagnosis, phenotyping and stratification. The consortium hopes to establish a multidisciplinary world-class centre that is driving the discovery, development, validation and adoption of non-invasive technologies to characterise disease signatures based upon the molecular analysis of breath.
About Leicester Precision Medicine Institute
The EMBER project forms part of the Leicester Precision Medicine Institute - one of four flag ship interdisciplinary Research Institutes that the University of Leicester has launched as part its strategic vision.
Future treatment of human disease will increasingly move from a ‘one size fits all’ approach to one of tailoring the treatment to the individual patient. Considering disease at a personal level allows for tailored (or precision) therapies where patient-specific responses are monitored and treatments refined to deliver optimal efficacy with minimal toxicity or adverse reaction.
The Leicester Precision Medicine Institute will coalesce and align the research missions of the university and the NHS in Leicester. This Centre of Excellence will develop, evaluate, and implement treatments based on individual patient differences, to provide better healthcare that recognises the ethnic diversity of our population. For more information, visit www2.le.ac.uk/institution/ilh/sub/stratified-medicine-within-the-respiratory-theme
Source: Owlstone Medical
