'Smart' Endoscope Provides Closed-Loop Solution For Colon Cancer
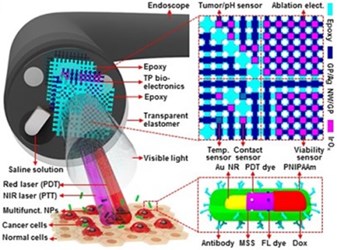
A new multi-modal endoscope developed at the Institute for Basic Science (IBS) in Korea is capable of both detecting small cancers and providing therapeutic interventions, such as laser ablation and localized chemotherapy. IBS scientists say the technology could pave the way for more personalized and precise treatments for patients with colon cancer.
Early endoscopes were snake-like tubes fitted with a light source and camera and were useful primarily as a diagnostic device for diseases and abnormalities of the gastrointestinal (GI) tract. Recent advances in the technology now allow surgeons to both find the problem and treat it over the course of one procedure, greatly reducing patient risk and suffering.
A recently published white paper states that one of the major drawbacks of conventional endoscopy is its reliance on white-light reflectance (WLR) and the subjective limitations of human vision. According to experts, these limitations can lead to under-diagnosis of dangerous cancers and missed opportunities for early intervention.
The IBS team noted in a press release that conventional endoscopes do not have the spatial resolution necessary to detect micro-scale tumors, and the technology has not been appropriately miniaturized to fit the maximum amount of function on a device that can safely navigate the GI system.
Their solution is a system that combines “transparent bioelectronics, such as lasers, with theranostic nanoparticles (NPs)” that are capable of “optical-fluorescence-based mapping, electric impedance and pH sensing, contact/temperature monitoring, radio frequency (RF) ablation and localized photo/chemotherapy,” said authors of a study published in Nature Communications.
Conducting in vivo experiments with mice, the team first injected the animals with NPs — preloaded with fluorescent dyes — that actively targeted colon cancer cells. Laser light on the endoscope located the cancer cells, which the scientists could ablate and dose with cancer-fighting drugs.
Researchers found that mice treated with the ‘smart’ systems saw their tumors significantly reduced, whereas tumors in the control group mice — which did not receive NP injections or cancer drugs — increased in size.
This system, said study authors, “has the potential to reduce the procedure time and improve the efficiency of minimally invasive surgical procedures for colon cancer treatment. Furthermore, efficient therapy can contribute to the excellent oncologic and economic yield for various GI cancers or precancerous lesions in the future.”
According to the American Board of Surgery, endoscopy is one the top five most common procedures conducted by American surgeons, due to its minimal invasiveness and broadening capabilities. Despite FDA regulations and federally mandated taxes, North America is projected to lead the endoscopy market through 2017, said a report by Transparency Market Research.
The CDC estimates that 134,000 patients are diagnosed with colon cancer each year, and over 50,000 of those cases are fatal.
